バイオプリンティングで糖尿病患者のQOL(生活の質)を向上させた医師の研究
成人の11人に1人が糖尿病であると言われています。これは全世界で4億2500万人以上であり、2045年には6億2900万人に増加すると予想されています(IDF, 2017)。
糖尿病を管理するために、多くの人は毎日インスリンを投与し、血糖値を測定する必要があります。糖尿病の人は、血糖値に気をつけるだけでなく、常に目標値を維持する努力が必要です。
糖尿病の管理は、まるでフルタイムの仕事のよう
糖尿病と上手に付き合うためには、1日に何度も自己注射したり指を刺したりする必要があります。糖尿病患者は、食べてもよいもの、食べてはいけないものを常に考えています。 心臓発作や脳卒中、失明、下肢切断などの糖尿病合併症を防ぐには、このような意識を常に持ち続けることが重要です。
糖尿病の管理に日々気を配ることには疲労を伴い、その結果、糖尿病バーンアウト(燃え尽き症候群)になることも少なくありません。最も意欲的な糖尿病患者でも、理想的な血糖値に達するのは半数で、その値を長期間維持できるのは5%未満です。一般の人と比べて、糖尿病を患うとうつ病のリスクが2倍になることは、驚くことではないかもしれません(Snoek and Skinner, 2006)。

糖尿病治療の未来
糖尿病を完治させる方法はありません。現在、糖尿病患者は、膵臓移植を受けるまでに何年もかけて病状を管理しています。その待ち時間が、Michał Wszoła医師を最も悩ませていることの1つです。
「移植を何年も待つことなく、患者が助かる方法があるはずです。糖尿病が刻一刻と自分の体を蝕んでいることを知りながら、一分一秒電話を待っているのです」と先生は仰いました。
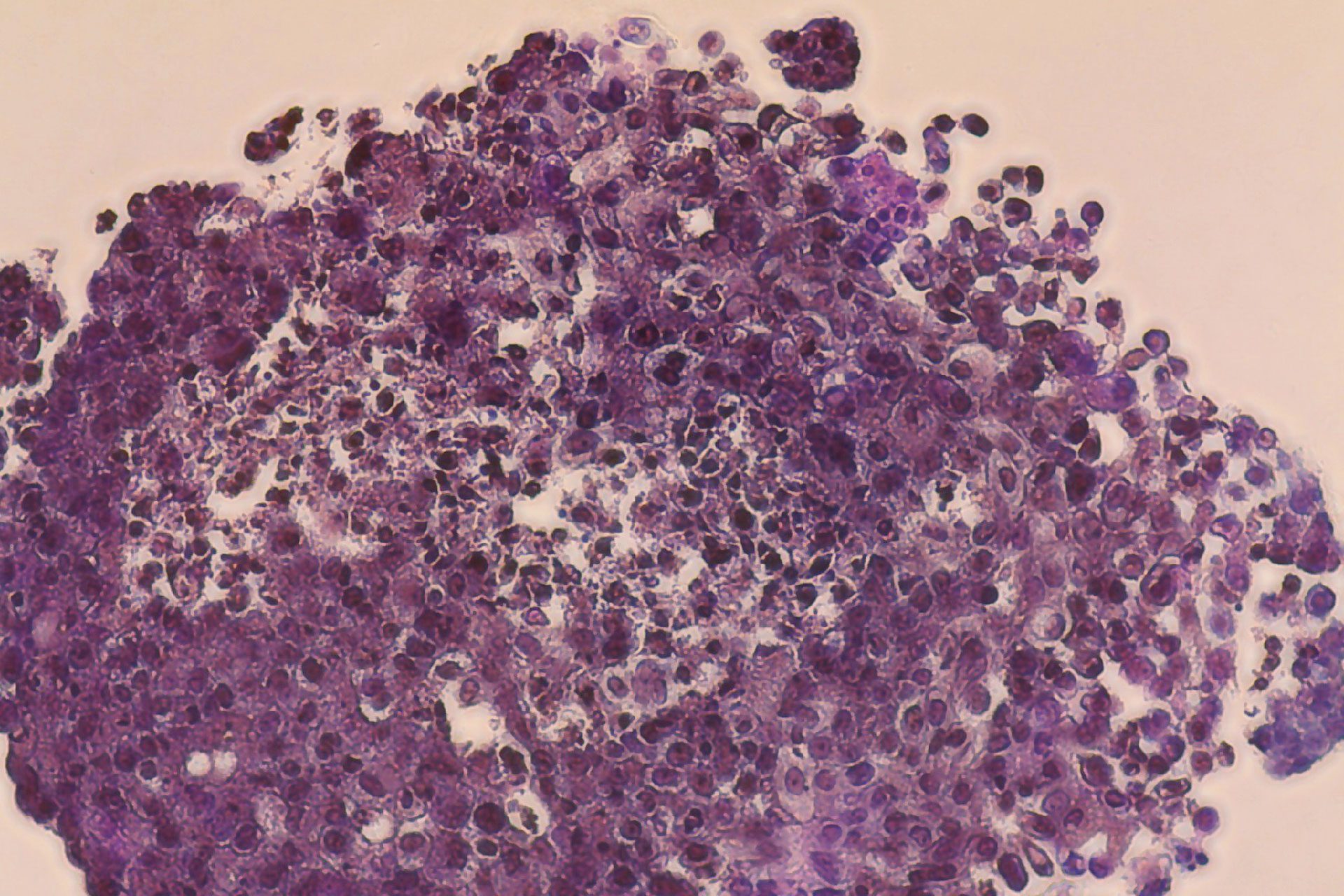
同時に、Wszoła医師は膵臓移植が最良の結果をもたらすことを知っていました。しかし、致命的な合併症を引き起こす可能性があるため、代わりに膵島を移植することに興味を持ったのです。いくつかの動物実験を行い、有望な結果を得ましたが、移植された膵島細胞に反応して起こるアポトーシス(自動細胞死)を防ぐ方法を見つける必要がありました。
「この課題を克服できるものはないか、私は探し始めました。アポトーシスや免疫抑制治療を避けながら、患者一人ひとりに合った臓器を提供できる低侵襲の治療法を開発したいと思いました。」
「色々と調べた結果、バイオプリンティングという非常に興味深い技術を知り、これらのハードルをすべて克服できる可能性があることがわかりました。」
バイオプリンティングでより良い治療を実現するために
コンソーシアムを立ち上げ、資金を受け取ると、Wszoła医師は、バイオプリンティングを活用した糖尿病治療法の開発を目指し、精力的に活動を開始しました。
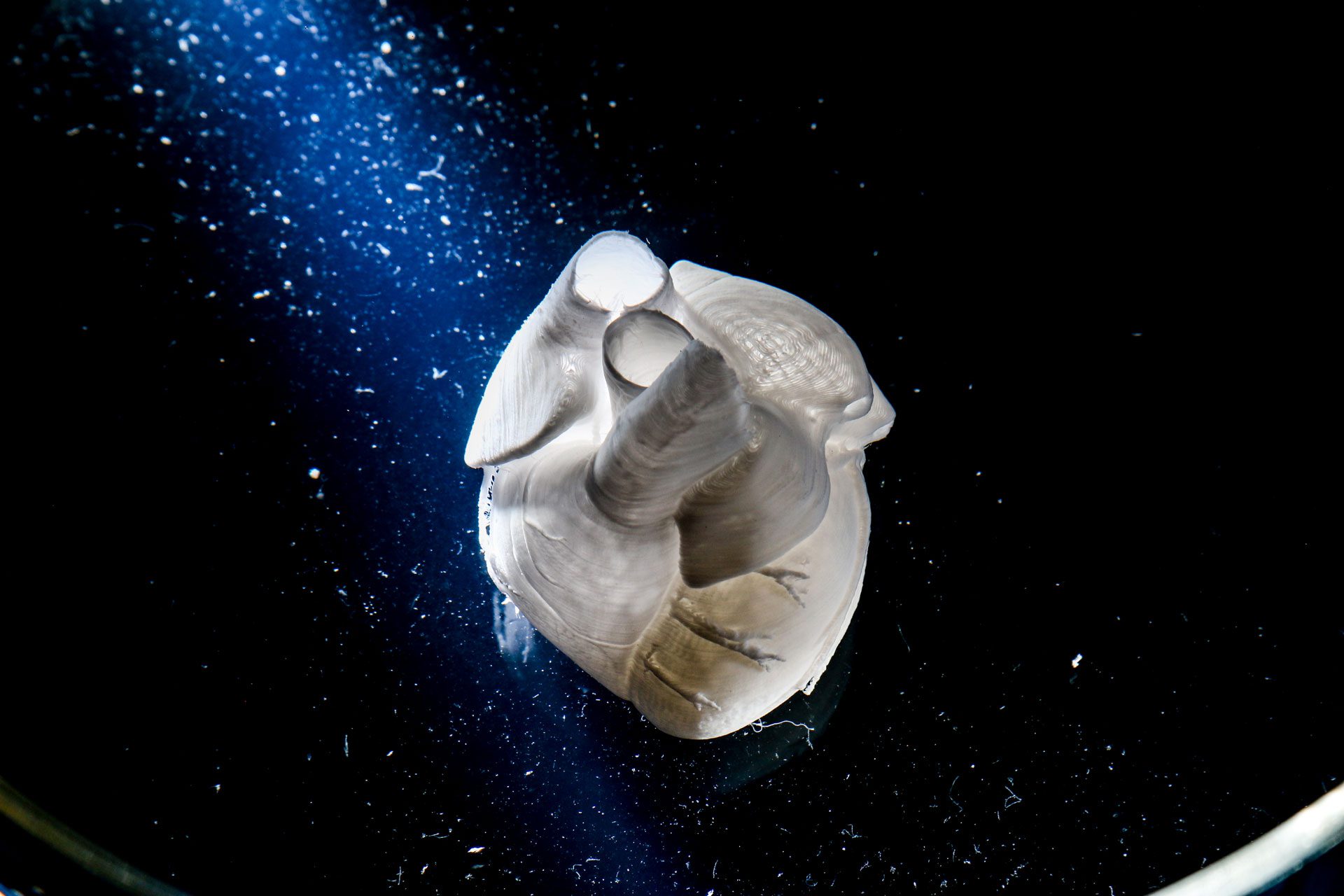
この革新的な技術により、Wszoła医師は有望な結果を得ることができました。3月14日、先生の研究チームは、テーラーメイドのバイオインクと膵島サンプルを使って、バイオニック膵臓のバイオプリントに成功しました。ブドウ糖刺激に対する反応は完璧で、さらに4回の実験を行い、同様の結果を得ることができました。

明るい未来は糖尿病以外の治療にも
Wszoła医師が開発している技術の有効性は、糖尿病だけではありません。この方法は、将来的には皮膚や膀胱、肝臓などの臓器をプリントするのに使われるかもしれません。これらのプラットフォームは、医薬品開発や新しいがん治療法のスクリーニングに活用できる可能性があります。Wszoła医師の研究が、製薬業界全体に大きな影響を与える日が来るでしょう。
では、次のステップは何でしょうか?
「現在、私たちはいくつかの課題に取り組んでいます。バイオニック膵臓が高圧に耐えられることを確認し、患者の体内の血管にバイオニック膵臓を接合する方法を考えなければなりません」とWszoła医師は語ります。
今後は、in vivoの動物実験や臨床段階への移行に注力する予定とのことです。